Cover Story: Cognitive Issues with Multiple Sclerosis: Research, Strategies and Support
By Susan Wells Courtney
Reviewed by Jack Burks, MD

Cognitive changes with multiple sclerosis (MS) are fairly common. Most studies state that approximately 50 percent of individuals with MS may have some type of cognitive dysfunction, although some estimates are as high as 60 or even 70 percent. Individuals with MS who experience cognitive issues may have trouble with functions such as attention, information-processing speed, executive functions (decision making), episodic memory, and visuospatial abilities. These deficits can affect several activities of daily living, including employment, driving, social integration, and adherence to medication regimens. Concentration and attention shifting are other examples of cognition impairments observed with MS.
The study of cognitive changes with MS is both extensive and varied, yet still in its early stages. A search of peer-reviewed articles reveals findings from hundreds of recent trials within the past few years, conducted in countries all over the world, and covering a wide range of objectives – from evaluating assessment tools and looking at cognition’s impact on quality of life, to identifying potential causes and determining the effectiveness of certain treatment strategies.
Why is the study of cognition in MS so complex? This is because so many variables exist with this symptom and its manifestations. For example, cognitive changes can be a difficult area to measure and to compare with controls. Researchers are looking for the optimal tests to best evaluate the presence, type, and severity of cognitive deficits in different individuals with MS. The variety of tests used in these trials is impressive; for example, these may include questionnaires, dual-task evaluations, measures of eye movements, computerized tests of cognitive function, an array of physical, mental, and emotional scales, several types of neuroimaging, and more.
DESCRIBING COGNITIVE DYSFUNCTION
Acclaimed author Jeffrey N. Gingold, writer of Facing the Cognitive Challenges of Multiple Sclerosis, Second Edition (Demos Health, 2011) and Mental Sharpening Stones (Demos Health, 2008), has been able to put into words exactly what it feels like to experience a sudden lapse in cognition, where familiar surroundings are no longer familiar, and wellversed words cannot be found.
In Facing the Cognitive Challenges of Multiple Sclerosis, Second Edition, Mr. Gingold talks about his work as a successful lawyer who is suddenly faced with a host of cognitive challenges, some of which arise at the most inopportune of times. At right are excerpts from the Preface of this book, touching briefly on his experience with cognitive issues from MS.
Another book written by Mr. Gingold, Mental Sharpening Stones, also provides detailed descriptions of sudden lapses in cognition. It goes on to give valuable direction and tips for managing this symptom. Other books are available on the topic of cognition and MS, including Multiple Sclerosis: Understanding the Cognitive Challenges, which is an excellent resource written by Nicholas LaRocca, PhD and Rosalind Kalb, PhD (Demos Medical Publishing, 2006). All three of these books, as well as others, may be borrowed at no charge from MSAA’s Lending Library. Please see page 48 for details about this helpful program.
“Without warning, many people with MS are suddenly faced with an inability to process routine thoughts. Their decision making may be stonewalled, befuddling simple conversations into a word-finding struggle. Others may lose their bearings in their own backyard or kitchen, or suddenly the face of a spouse or friend will appear unfamiliar. Then, the shroud over their memory recall lifts, defying explanation, and leaving no trace of the bait and switch. The individual’s cognitive functions have been compromised and often go undiagnosed, creating a deep chasm of unseen disability.”
– Jeffrey N. Gingold,
Facing the Cognitive Challenges of
Multiple Sclerosis, Second Edition
Even with all of these tools, many questions still remain. For instance, when an individual with cognitive issues provides self-reported evaluations, are these answers valid? The findings from a study in France suggest that cognitive dysfunction did not compromise the reliability or validity of one’s responses on quality of life questionnaires, but these types of issues need to be considered when conducting studies on the effects of cognitive problems. Further complicating this issue is the fact that medications used for symptom management may also affect cognition as a side effect, and this too must be included in the equation.
Neuroimaging is vital in determining what specific areas of the brain may be affected by MS to cause cognitive problems, as well as parts of the brain that may compensate for areas that are no longer conducting nerve impulses efficiently. Many forms of imaging technology are used for this purpose and can provide important data to researchers, enabling them to theorize the different areas of the brain that may impact cognition. Some of these types of tests are used to observe the activity in parts of the brain while a patient performs a task, and these data may be compared to someone without cognitive issues performing the same task.
Additionally, the type or stage of MS can exhibit different types and degrees of cognitive changes. Researchers are studying both relapsing and progressive forms of MS, as well as individuals with clinically isolated syndrome (CIS) and pediatric MS. Studies are also being conducted to determine if other symptoms may impact cognition, such as depression and other changes in mood, fatigue, poor sleep, and more. And perhaps the biggest variable in evaluating cognitive issues in MS is the day-to-day variations in symptoms as well as during times of exacerbations or pseudo-exacerbations.
Demographics are another area of interest, and in this category, gender may even play a role. A Spanish study found that gender may have an impact on cognitive performance, and in this instance, found that males with MS exhibited poorer cognitive performance, largely in terms of verbal auditory memory. However, a study in Finland found that male patients with severe attentional deficits benefited more from neuropsychological intervention, as compared to females in the study. Much remains to be learned about this challenging symptom, and as illustrated in this example, a variety of outcomes may be derived from this research.
As researchers delve further into the effects of cognitive issues in MS and look to find the causes, another important area of study is that which evaluates the effectiveness of potential treatments. Different forms of exercise as well as various types of cognitive training/ neuro–psychological rehabilitation are two areas of potential treatments that are being studied closely.
Many trials are also underway to look at the effectiveness of the different approved and experimental disease-modifying therapies in delaying, improving, or preventing cognitive symptoms. Other treatments, such as fampridine, statins, and vitamin A, are now including changes in cognition among their study endpoints.
The many variables mentioned above are just examples of the great complexity involved with learning about and treating cognitive dysfunction in MS. In the pages to follow, this article will provide excerpts from published studies from around the world, aimed at evaluating this challenging symptom and its potential causes, along with various treatment strategies. Readers may also learn about current studies and hear from two professionals who work closely with individuals experiencing cognitive issues from MS.
Changes in the Brain That May Lead to Cognitive Problems
Causes of Cognitive Symptoms
Descriptions and Makeup of the Brain
What leads to cognitive problems in MS? Changes in the brain caused by damage to the myelin and axons (nerves in the brain) are the primary cause of cognitive dysfunction in MS. Research is ongoing to identify the exact locations of damage that cause cognition issues in individuals with MS. Additionally, damage to different locations of the brain affect different types of cognitive function, such as attention, information-processing speed, executive function, and memory, to name a few. The hope is that through such studies, treatments may eventually be designed to target these areas and minimize or prevent any effects that MS may have on cognition.
The term “cognition” refers to a group of mental processes such as information processing, language, memory, visual perception/spatial skills, calculation skills, and executive functions (LaRocca, Sorenson and Fischer, 2000). These may be described as follows:
- Information-processing skills affect our ability to focus, maintain, and shift our attention from one thing to another without losing track of what we were doing, as well as managing incoming information quickly.
- Language refers to the ability to understand and use language appropriately in daily situations.
- Memory is a complex set of skills that involve learning, storage of information, and the ability to retrieve that information on demand.
- Visual perceptual/spatial skills allow us to do things such as recognize objects, draw, assemble things, and find our way around.
- Performing simple and complex math skills are involved in calculation abilities.
- Executive-functioning abilities enable us to get through our day by overseeing and coordinating tasks such as organization, planning, sequencing, problem solving, judgment, reasoning, monitoring our own behavior, etc.
The most commonly affected cognitive processes in MS are speed-of-information processing, memory, and executive functions. Other domains of cognition can also be affected depending on where lesions are located. However, rarely are all domains of cognition impacted by MS.
Glossary of Terms
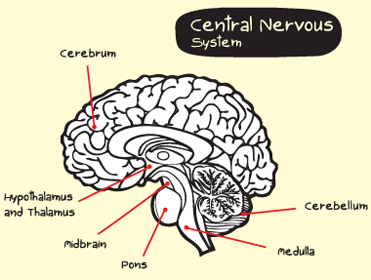
Basal ganglia and thalamus
These are structures at the base of the brain composed of nerve cells; they are responsible for body movements and coordination. They also function as a relay center for sensory impulses to the cerebral cortex. Damage in this area may cause cognitive problems.
Brain atrophy
A wasting or decrease in size of part of the brain because of disease, such as MS.
Brainstem (midbrain, pons, and medulla)
Brain structure connecting the cerebrum pathways to the spinal cord, which leads to nerves in the arms and legs. It also controls vital functions, movement, sensation, and nerves supplying the head and neck.
Cerebellum
The cerebellum is at the base and the back of the brain. The cerebellum is responsible for coordination and balance.
Cerebral cortex/gray matter
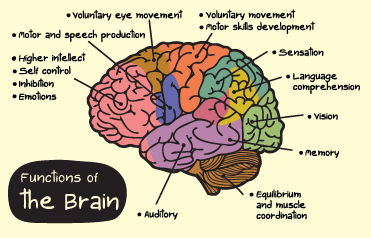
This is the outer gray matter of the cerebrum, where many of the higher functions, such as volition, consciousness, conceptualization, motor activity, speech, and sensation, are carried out. This gray matter is mainly composed of nerve cells.
Cerebrum
This is the large, top portion of the brain that is divided into four lobes and is joined at the bottom by the corpus callosum. It controls and integrates motor, sensory, and higher mental functions, such as thought, reason, emotion, and memory.
The four sections of lobes that make up the cerebrum are:
- The frontal lobes that are responsible for problem solving, judgment, and motor function.
- The parietal lobes that manage sensation, handwriting, and body position.
- The temporal lobes, including the hippocampus and limbic system, are involved with memory and hearing.
- The occipital lobes that contain the brain’s visual processing system.
Corpus callosum
Part of the cerebrum, this is a plate of nerve fibers connecting the two cerebral hemispheres, except for most of the temporal lobes.
White matter
Areas of the nervous system composed mostly of myelinated nerve fibers (those having myelin sheaths) that conduct nerve impulses.
Please note that portions of the information appearing in this article are described in “Cognition, Cognitive Dysfunction, and Cognitive Rehabilitation in Multiple Sclerosis,” written by Pepping M, et al, Phys Med Rehabil Clin N Am 24 (2013) 663-672.
Both acute inflammatory demyelination and axonal degeneration are thought to be the primary causes of MS-related disability. Although MS is often considered to be a disorder affecting only subcortical white matter, considerable evidence has shown that cortical demyelination can also occur, even at early stages of disease. Since both subcortical and cortical brain regions appear to be affected, this indicates that the nature of MS is diffuse (spread over a wide area), and may explain why a widespread set of cognitive issues are possible.
What is notable about this data is the fact that MS damage leading to disability was at one time thought to be limited to white matter. The axons (nerves in the brain) found in white matter are insulated by myelin, which is the primary target of MS damage. However, when MS damage extends to the gray matter – consisting of dense nerve cells and myelin that is less apparent – additional disability, including cognition, can be affected. Gray matter damage is usually more widespread than the more well-defined white-matter lesions. This is why damage going beyond the white matter and extending into the gray matter is often referred to as “diffuse.”
According to the authors of this article, despite the potential for diffuse brain involvement, MS lesions tend to locate in white matter, the cerebellum, and the brainstem. White-matter lesion load (or burden), the location of the lesions, and the amount of global or regional brain atrophy – which is the shrinking or reduction in brain volume – are of greatest interest in the study of cognitive dysfunction in MS. To follow are some examples of MS damage and the type of cognitive functions that they affect:
- Lesion load in areas near the cortex may cause problems with memory
- MS damage in the frontal lobe can affect executive function (which includes judgement and problem solving)
- Global and regional brain atrophy is particularly associated with cognitive dysfunction
Additionally, in some studies, brain atrophy (reduction in tissue) was found to contribute more to cognitive impairment than the degree of lesion load. Other examples of damage that appear to affect cognitive function include:
- The width of the third ventricle, which was more highly associated with cognitive dysfunction than whole-brain (overall) atrophy
- A central role of the thalamus is to act as a relay station for the transmission of information between different areas of the brain; this could explain why atrophy in these areas has significant effects on key frontal-subcortical functions, which include thought and memory
- In some studies, cognitive impairment and atrophy of the thalamus were particularly linked to men – although the reason for this is not known
To follow are a few brief findings from recent studies, which suggest that different areas of the brain may to play a role in cognitive symptoms with MS. As readers can see, researchers have differing opinions as to what areas or factors have the greatest impact on cognitive functioning. These reports are just a sampling of the many studies that have been published within the past few years.
A study from Buffalo, New York states that there is a well-established correlation between deep gray matter atrophy and cognitive dysfunction in MS. The study’s findings also suggest that iron accumulation in the thalamus may play a role in MS cognitive decline.
An international study reports that changes in the basal ganglia, such as the thalamas, are related to mobility and cognitive impairment.
A study from Cleveland, Ohio indicates that in patients with MS, hippocampal volume (the hippocampus is part of the temperal lobe in the cerebral cortex) was related to reduced memory and information-processing speed. These results highlight the role of the hippocampus in cognitive dysfunction in patients with MS and suggest that measures of hippocampal atrophy could be used to capture aspects of disease progression.
A study in Switzerland indicates that cerebellar abnormalities can contribute to disability, including cognitive impairment in MS.
Researchers in the United Kingdom linked Glutamate, an excitatory neurotransmitter, with memory problems.
Researchers in Canada report that they investigated the association between cognitive impairment and white matter dysfunction in secondary-progressive multiple sclerosis.
Other Factors that May Play a Role in Cognitive Problems in MS
Other factors may be involved with the cognitive symptoms of MS. To follow is a listing of some of these factors that have been hypothesized or implicated in recent studies.
Isolated Cognitive Relapses: From a study conducted in several countries, “While cognition can be affected during sensorimotor multiple sclerosis (MS) relapses, the relevance of isolated cognitive relapses (ICRs, i.e., those occurring in absence of new sensorimotor symptoms) remain poorly characterized. Here, we decided to explore the relationship between ICR, subjective evaluation of cognitive performance and long-term cognitive decline in a group of subjects with relapsing-remitting MS… Subjects who presented with an ICR [at six months into the study] presented with a significantly reduced cognitive performance at the follow-up evaluations compared with patients without ICR.”
Polypharmacy (use of multiple medications): Researchers in Kansas City reported that patients with multiple sclerosis (MS) commonly use a variety of medications to slow disease progression, alleviate symptoms, and treat comorbid conditions. The use of multiple medications (polypharmacy) can be associated with additional fatigue and memory problems. The investigators recommend that patients and healthcare professionals weigh the risks and the benefits of using multiple medications at one time, given the potential for a possible increase in fatigue and cognitive issues.
Smoking: Investigators in Istanbul, Turkey explain, “According to the results of our study, heavy smokers had increased cognitive impairment when compared to nonsmokers. Extensive studies are necessary to further elucidate the relationship between smoking and cognitive impairment in MS patients.”

Gut microbiota: Italian researchers suggest that the potential relationship with bacteria in the GI tracts and their potential influence on the immune system in neurological disease (such as MS), with an impact on pain and cognition. Mutual impact of gastro-intestinal tract (GIT) and central nervous system (CNS) functions has been recognized since the mid-twentieth century. They studied how the commensal gut microbiota influences systemic immune response in some neurological disorders, highlighting its impact on pain and cognition in multiple sclerosis. To follow are some recently reported study findings, helping to provide a broader understanding of the impact and variables in cognitive dysfunction as a symptom of MS, as well as help to identify the most useful methods of assessment.
ADDITIONAL RECENT STUDY FINDINGS
To follow are some recently reported study findings, helping to provide a broader understanding of the impact and variables in cognitive dysfunction as a symptom of MS, as well as help to identify the most useful methods of assessment.
Assessment Tools
A German study explains, “Patients with relapsing-remitting multiple sclerosis and age-and gender-matched healthy individuals were tested with common neuropsychological tests and a computer-based visual search task, whereby a target stimulus has to be detected amongst distracting stimuli on a touch screen… [The researchers concluded that] visual search is a promising instrument for the assessment of cognitive functions and potentially cognitive changes in patients with multiple sclerosis thanks to its good discriminatory power and insusceptibility to practice effects.”

Cognitive rehabilitation (discussed later) encourages people with cognitive issues to stay active and employ helpful strategies. These strategies include planning ahead and using written notes – both for memory prompts and for increased organization.
In Kansas City, Missouri, researchers explain, “Eye movement difficulties in multiple sclerosis (MS) are common and may influence performance on cognitive tests… [Two] studies examined associations between a new measure of speedy eye movement and visual/nonvisual cognitive tests. In both studies, slower eye movements were significantly associated with poorer performance on cognitive tests… Pending further research, the Speedy Eyes Test [SET], a brief, inexpensive, and nontechnical measure of speedy eye movement, may serve as a visual/oculomotor indicator of cognitive impairment in multiple sclerosis.”
Dual Tasks of Walking and Cognition
The University of Illinois report that performing a cognitive task, while walking, results in a reduction of walking performance among persons with MS. Any loss in function that occurs because of doing two tasks at one time is referred to as dual-task cost, or DTC. Study investigators examined walking performance, cognitive processing speed, and symptoms of fatigue, depression, anxiety, and pain as correlates of DTC of walking in MS. There were significant and large declines in gait performance with the addition of a cognitive task for velocity, cadence, and step length. Walking performance might be a target of interventions for reducing the DTC of walking in MS.
TREATMENT STRATEGIES FOR COGNITIVE SYMPTOMS IN MS
As noted earlier in this article, at least 50 percent of individuals with MS experience changes in cognition. This is often a challenging symptom that can impact one’s life in many ways. For instance, some individuals with cognitive issues may reduce or discontinue their participation in outside activities, they may become less socially active, and employment is often affected.
At home, problems with cognition can also affect one’s ability to perform everyday activities, as routine duties may take longer to complete, things may be forgotten, and stress may arise over these changes. Other symptoms of MS, such as fatigue and depression, may have a negative impact on cognition as well.
Treatment options and studies into potential new treatments are of constant interest and concern to the MS community. In this section, the possible benefits of exercise, medications, and cognitive rehabilitation are discussed.
Studies into Exercise and Cognition in MS
Common Questions and Answers Regarding Cognitive Issues In MS

Mrs. Angel Blair, M.A. is one of MSAA’s Client Services Specialists. When asked about cognition as a symptom of MS, she talked about the experiences she has had with callers to MSAA’s Helpline. First, Mrs. Blair provided examples of client calls and inquiries that she often receives in regards to this symptom. Common questions include:
Can MS affect cognition, memory, or judgment? Clients may report forgetfulness, not thinking as clearly or quickly as they once did, feelings of being overwhelmed, and not knowing if this is a symptom caused by their MS.
Are there ways to manage or treat this
issue? Clients ask what they can do about these symptoms and who they can see for it.
Will MS affect their thinking? They want to know if this is something that will occur in the future.
Next, Mrs. Blair provided the types of information that she and other Client Services Specialists provide in response to these inquiries, as follows:
MS can have the ability to affect one’s cognition – thinking, memory, decision making, and judgment – especially in relation to where the disease is causing damage and inflammation in the brain. Other MS-symptom issues can also affect one’s cognition, and these might include fatigue, problems in sleep management, and depression. The side effects of medication can also have an impact on cognition. Other factors that affect cognition include anemia, infection, and thyroid problems. This does not necessarily mean that every individual with MS will experience this symptom, as everyone’s experience and symptom presentation with MS differs, but it is something that can occur as a challenge in the disease process.
Evaluating and considering all factors that could be involved in the appearance and/or worsening of this symptom is important, as other health conditions can occur in conjunction with MS and may be a contributing factor to difficulties in thinking or processing information. Talking to one’s doctor can help to distinguish the cause of these changes.
In regard to symptom management and evaluations for cognitive issues, the first step would be to work with his or her neurologist in discussing what these symptoms are, what’s been noticed, what types of changes have occurred, and any other concerns one may have.
A neurologist may want to recommend baseline cognitive evaluations and testing, perhaps with the support of a neuropsychologist, who is a specialist focusing on mental processes, behavior, and thinking as they relate to the structure of the brain. This type of doctor can perform different types of testing in regards to one’s current rate of processing thoughts and tasks. This testing can include a series of different tests to evaluate language, memory, organization, and similar types of functions.
After an evaluation, the specialist may then recommend and work with a client to create some type of cognitive rehabilitation treatment plan. This would include identifying problem areas and working on strategies for improvement in processing. Among other methods, this can include specific tasks and activities, games, exercise, and those types of things, all tailored to meet the client’s specific needs.
Mrs. Blair also notes the possible impact that cognitive issues may have on daily life:
Cognitive challenges can interfere with daily tasks, such as household duties and responsibilities. For instance, memory issues and forgetfulness can cause problems when trying to complete chores or errands, making and keeping appointments, staying organized, and performing other daily activities.
Cognitive issues can impact one’s employment and job responsibilities, if memory and forgetfulness start to interfere with the completion of tasks. Decision making on the job can also be affected if one’s judgment and executive function are at all compromised.
Management strategies may be developed to help someone who is having trouble at work as a result of cognitive problems caused by MS. Asking for accommodations in the workplace, if needed, can be very helpful. Another option is to take advantage of vocational rehabilitation services. These are specific counseling and employment-related services for those with disabilities – to identify areas of need and ways to manage and improve upon this issue.
Making lists, using files, or employing other organizational methods that help to keep things in order, both at work and a home, can assist individuals in accomplishing tasks and minimizing the effects of forgetfulness and other cognitive issues. If appropriate and as needed, asking for help to delegate tasks to others can be very helpful as well.
Communication is key. This includes having conversations with one’s healthcare team and his or her family or support network to discuss cognitive issues, ways they can be managed, recommendations for treatment, and obstacles that may be modified to accommodate for these changes.
Cognitive difficulties can be a very sensitive and complicated issue to discuss with others, but it’s important for individuals with MS and their families to know that they are not alone and there are supports in place to help people cope with this symptom.
With or without MS, the positive effects of exercise on cognition are frequently mentioned in the news. The following data provide interesting information on different types of exercise when studied in individuals with MS and their effects on cognitive function.
Researchers from an Illinois study explain, “The current study compared the acute effects of moderate-intensity treadmill walking, moderate-intensity cycle ergometry, and guided yoga with those of quiet rest on executive control in 24 persons with relapsing-remitting MS without impaired cognitive processing speed… The present results support treadmill walking as the modality of exercise that might exert the largest beneficial effects on executive control in persons with relapsing-remitting MS without impaired cognitive processing speed. This represents an exciting starting point for delineating the appropriate exercise stimulus (i.e., modality and intensity) for inclusion in a subsequent longitudinal exercise training intervention for improving cognitive performance in this population.”
Investigators from Seattle report, “The present study adopted a randomized controlled trial design and examined the effect of a physical activity behavioral intervention on cognitive and walking performance among persons with MS who have mild or moderate disability status… The current study supports physical activity as a promising tool for managing cognitive impairment and impaired walking performance in persons with MS, and suggests that physical activity might have specific effects on cognition and non-specific effects on walking performance in this population.”
Research in Seattle has also set out “to determine whether there is an association between improvements in objective measures of physical fitness and performance on cognitive tests in people with multiple sclerosis (MS)… Participants in the physically improved group demonstrated improved performance on measures of executive functioning after 12 weeks of exercise. The results of this study lend support to the hypothesis that change in fitness is associated with improved executive functioning in people with MS.”
Canadian researchers have found, “Exercise may have beneficial effects on both well-being and walking ability in multiple sclerosis (MS). Exercise is shown to be neuroprotective in rodents and may also enhance cognitive function in humans. It may, therefore, be particularly useful for MS patients with pronounced neurodegeneration…
“Patients with progressive MS and moderate disability were randomized to one of three exercise interventions (arm ergometry, rowing, bicycle ergometry) for 8-10 weeks or a waitlist control group… Significant improvements were seen in aerobic fitness. In addition, exercise improved walking ability, depressive symptoms, fatigue and several domains of cognitive function. This study indicated that aerobic training is feasible and could be beneficial for patients with progressive MS. Larger exercise studies are needed to confirm the effect on cognition.”
Treatments with Medication
As discussed in MSAA’s Winter/Spring 2013 issue of The Motivator, one of the best ways to maintain cognition is to do your best to avoid new lesions by taking a disease-modifying therapy (if you have a relapsing form of MS). A number of studies with these drugs have shown some benefit on protecting cognition. Twelve disease-modifying therapies are now approved for use by the United States Food and Drug Administration (FDA) for relapsing forms of MS. Please visit MSAA’s website at mymsaa.org for specific information on these approved therapies.
People with MS and MS clinicians have hoped that medications such as those that help people with Alzheimer’s disease might also benefit people with MS. Some of the Alzheimer’s disease medications work to block the enzyme that breaks down the nerve signal messenger acetylcholine. Although early reports suggested that the medication Aricept® (donepezil) might help cognition in MS, more thorough research has not proven this drug to be of benefit.
Additional studies of the Alzheimer’s medications Exelon® (rivastigmine) and Namenda® (memantine HCl) also did not demonstrate a clear benefit. Some side effects may include stomach or bowel problems, mood changes, and urinary difficulty. Others had hoped that the herbal extract ginkgo biloba would be of benefit, however, preliminary studies have not demonstrated a benefit. Many other supplements are often promoted to help memory in the general population, but hard data is very limited even for people without MS. Be sure to discuss any drugs or supplements you may be taking with your healthcare team.
Treating fatigue may reduce its effects, but does it help memory? This is a difficult area to study due to the difficulties in measuring and documenting cognitive changes, as well as the subjective nature of fatigue management. Small trials of amantadine (previously Symmetrel®) used for fatigue have not been convincing for cognitive improvement. The medication Provigil® (modafinil) and Nuvigil® (armodafinil) are commonly used “off label” for MS fatigue and have also been used by some with attention disorders. Ampyra® (dalfampridine), studied in the 4-aminopyridine form also did not demonstrate improvement. Management of fatigue by both pharmacologic and non-pharmacologic means may be tried by some, and may include occupational therapy for energy-conservation techniques.”
Several medications are currently being evaluated for the treatment of cognitive dysfunction in MS. Many of the approved DMTs have ongoing studies to determine their effectiveness in reducing cognitive challenges. Other medications and supplements are in study phases as well. To view current studies in this area of research and possibly look into participating in a clinical trial, readers may visit clinicaltrials.gov and search for “cognition and MS” for a full listing of related studies.
Cognitive Rehabilitation and Retraining

This area of work is showing much potential for improvement in cognitive symptoms. Investigators and clinicians are able to address each type of dysfunction with various approaches to help people improve or compensate for any cognitive challenges they may experience.
Cognition covers several different areas or patterns of function. In general, these categories include: attention, memory, acquisition and retrieval, information-processing speed, and executive function. The type and severity of cognitive dysfunction that an individual with MS experiences is largely dependent upon lesions occurring in certain regions of the brain, as well as areas of brain atrophy. Both the number of lesions (referred to as lesion load or burden) and atrophy (the shrinking of tissue or decrease in activity) are identified through neuroimaging techniques, such as a magnetic resonance imaging (MRI).
As mentioned earlier, a great deal of research continues to identify the specific areas of the brain that are affected by MS and lead to cognitive problems. Some studies have shown that brain atrophy, both regionally and globally, may contribute more to cognitive issues than the number of lesions. Noting that several areas of the brain may be affected, the effects of MS are thought to be widespread, and as a result, cognitive symptoms may be varied.
For this reason, cognitive rehabilitation specialists must conduct an extensive evaluation of their patients prior to and throughout the time they are in cognitive therapy. This enables the specialists to design the most appropriate treatment plans for their clients, and to revise these plans as needed throughout the rehabilitation period.
Initial Assessment for Cognitive Rehabilitation
An assessment or evaluation of the individual seeking treatment will include many important details, such as which types of neurocognitive symptoms (such as memory-retrieval problems) and neurobehavioral symptoms (such as reduced awareness and problem-solving issues) he or she is experiencing. Additional details include test data, background information from the patient’s neurologist or other treating physician, and historical information providing details about the individual prior to diagnosis.
The cognitive rehabilitation specialist will also note the patient’s reactivity to emotional concerns, as well as other symptoms that may have an impact on cognition (such as fatigue and pain). Identifying one’s abilities and preferences, along with learning about how he or she performs at school or at work, and in social situations, are also important while creating a customized treatment plan. Some of this information may be obtained through the family members and other individuals who are close with the patient. These people can also provide updates, letting the therapist know how the individual is doing in terms of applying the strategies and if any additional issues have been noted.
Additional testing may be required to help with the treatment plan. An occupational therapist may assess an individual’s ability to perform activities of daily living. A speech-language pathologist may look for any deficits in areas of communication. Learning what the person with MS is able to do and what problems he or she may have is critical to the initial assessment.
Many of the techniques used for cognitive rehabilitation and retraining in MS originated with those used to assist individuals with traumatic brain injury (TBI). While the two conditions differ in many ways and the severity of symptoms can vary greatly within either disorder, the same theories may be applied to the similar challenges of cognitive dysfunction. Whether the goals are to provide prompts that help with memory, to clear away distractions to increase attention, or to create more structure to improve executive function – or all three, along with many other strategies – these types of treatment plans are vital to improving one’s cognitive performance and ultimately increasing one’s quality of life.

Q&A
with a Speech Language Pathologist
Carrie Bruce, PhD, CCC-SLP
Senior Research Scientist, Center for Assistive Technology and Environmental Access at Georgia Tech
Member, MSAA Healthcare Advisory Council
What type of therapist(s) can assist with the diagnosis and treatment of cognitive issues with MS?
“When an individual with MS is experiencing some type of cognitive dysfunction, he or she would most often contact a clinical psychologist, neuropsychologist, occupational therapist, and/or speech-language pathologist.”
In general, how often might someone need to see a therapist, and does insurance usually pay for such appointments?
“It really depends on the focus of treatment, but most often cognitive rehabilitation works best when people participate on a frequent basis. The challenge in providing services is that it mostly results in few options for insurance coverage. Most insurance companies do not cover cognitive rehab services for people who experience deficits as a result of a non-acute neurological condition, including chronic diseases such as multiple sclerosis (and others such as congestive heart failure, autism, cerebral palsy, chronic obstructive pulmonary disease, or post chemotherapy). The research on the effectiveness of cognitive rehabilitation for MS that is used for coverage determination with most of the insurance companies reflects that it is experimental or that it does not have enough evidence to demonstrate medical necessity.”
Do you have any personal thoughts or guidance that you would want to give anyone with MS who may be experiencing cognitive issues?
“I would recommend for the individual to have a discussion with his or her medical provider first to review the list of medications to determine the impacts these may have on cognitive function. The medical provider can also discuss other potential sources of cognitive issues, such as nutritional deficits, poor sleep habits or sleep disorders, stress, etc. Individuals should be sure to talk with their medical provider before trying any alternative supplement that promises improvement in memory or other cognitive function. People experiencing cognitive issues should still try to maintain social connections and outlets that keep them mentally active and challenge their memory, attention, language, and problem-solving abilities.”
Strategies for Problems with Memory and Learning
Although occasional forgetfulness, difficulties recalling specific names, or losing things is fairly common, real problems with memory and learning can become a huge hurdle in accomplishing tasks, succeeding at school or work, and even accomplishing activities of daily living. For some people with MS, the ability to sift through several ideas and identify the most important ones becomes significantly affected. These individuals may then be greatly challenged to recognize what needs to be remembered and then be able to store this information so it is easily retrievable when details need to be recalled.
One of the best methods for improving memory is to take notes; the value of doing so can’t be overstated. Notes should be taken wherever and whenever information needs to be remembered – and this can include doctor appointments, school and work, at home, and while performing various activities such as shopping or attending meetings. The notes should be well-structured and kept in the same location, so they can always be immediately accessed.
Developing a system is important to make note-taking a part of the routine, and prompts should be included for both taking and reviewing notes regularly. Using a Day Planner-type of booklet or smartphone is ideal for keeping things organized. Dividing the information into smaller sections and practicing by re-reading and/or reading aloud helps to better store the information and enable one to retrieve the information when needed.
Improving Information-Processing Speed
When information cannot be processed quickly, many functions such as social interactions and day-to-day activities are affected. Having a conversation can become labored and uncomfortable; trying to follow directions can at times be almost impossible; and having to think of more than one or two concepts at the same time can lead to frustration and confusion. Fortunately, people who experience reduced information-processing speed may take steps to help minimize the effects of this type of dysfunction.
Consciously increasing one’s attention on the task, on the person speaking, or on whatever the event may be, while reducing any distractions, are good first steps (strategies for improving attention are noted in the next section). Another helpful tip is to take notes and ask questions – when appropriate – to assist with comprehension and understanding.
Additionally, using different forms of communication to reinforce the same information can also assist with speedier comprehension and retrieval. This might include seeing things visually (through attending an event, as well as viewing videos, charts, outlines, etc.), hearing the information presented either in person or on a recording, and written information, which includes asking people to email main points as a follow-up to a lecture or reviewing notes from the event.
Addressing Issues with Attention
Without the ability to focus and provide uninterrupted attention, one’s ability to listen, learn, and retain information is immediately compromised. Perhaps the most important strategy for improving attention is to reduce or eliminate any distractions. This may be accomplished by looking at the area where attention is needed and evaluating potential distractions. Whether they consist of sight or sound – necessary steps should be taken to reduce or eliminate these diversions. Examples include cleaning away extra clutter from a room, reducing the number of people present during a gathering, and/or turning off the TV and other electronic devices. Earplugs or headphones may also be used if needed to reduce noise or other competing distractions.
Sometimes people have thoughts that interfere with attention to the matter at hand. With this type of distraction, a good plan is to write down any ideas that might be monopolizing one’s thoughts and try to set them aside to focus on at a later time.
Attention may also be improved through identifying, organizing, and scheduling tasks and activities. This type of cognitive rehabilitation enables someone to perform daily functions efficiently and minimize how often he or she needs to shift attention to switch directions or return to repeat an action.
Improving Executive Function
Instruction on how to become better organized and step-by-step plans on how to start and complete projects are key strategies for improving one’s ability to employ good judgement and be able to solve problems efficiently. Structuring one’s schedule with reasonable timing to complete different projects can help to avoid becoming overwhelmed with everything that needs to be done.
To reduce the pressure of working under a tight deadline, individuals may want to double or triple their estimate of time required, just to avoid any extra stress. This is partly due to the fact that people with MS sometimes feel that their sense of time is diminished, and duties might be more time-consuming due to fatigue and other factors. Scheduling time to work when interruptions are at a minimum is also important.
Individuals with MS who experience problems with executive function need to be flexible with their schedule. While staying on track is worthwhile, people with MS need to be prepared for changes in symptoms that may disrupt their plans for the day, week, or potentially longer. Even when not experiencing any type of changes in symptoms, schedules should be regularly re-evaluated and revised as needed. Individuals should also be aware of their own physical limits as well as the fact that they may be more easily distracted now than prior to their diagnosis.
Increased Awareness and Continued Learning
Individuals with MS who are experiencing cognitive difficulties may benefit greatly by staying aware of their limitations and continually learning new ways to counter the effects of this challenging symptom. Through the knowledge that cognitive issues could be slowing them down, causing frustration and forgetfulness, as well as other implications, individuals may be empowered by regularly learning and employing new techniques. Doing so can lead to a better quality of life and even greater success with their endeavors.
Furthermore, relationships may become more positive as plans are put into place to counter any problem areas. Other urgent responsibilities, such as taking one’s medications at the correct times and dosages, may be more closely followed through planning, organization, and the added attention the individual knows is necessary.
Closing Notes
When asked about cognitive problems experienced by people with MS, MSAA Chief Medical Officer Jack Burks, MD, reflects on the many challenges that some individuals with MS may face while coping with this often unexpected symptom. At the same time, he is pleased to explain that several proven strategies, as well as new and emerging therapies, are becoming available, all of which may provide the help needed to counter these types of symptoms.
Dr. Burks explains, “Many people with MS tend to focus on their physical challenges and minimize or deny their cognitive issues, although they may realize some difficulties at work, at home, or with social interactions. Their adherence to MS medications may also suffer.
“When finally evaluated by neuropsycho-logical testing, they are often surprised by the degree of difficulties they experience during the tests. They often believe that if they look and feel ‘pretty good,’ drive safely, get satisfactory job performance evaluations, and can handle their checkbook, they must not be cognitively impaired. Once the problem is identified, they are initially upset. However, after they learn how to deal with the issues, they are relieved by the ability to accomplish even more.
“The bottom line is that cognitive problems may exist… but so do many opportunities and strategies that are available to help people perform their cognitive tasks. This article provided insights into the enormous research efforts related to MS cognition and ideas to improve one’s daily living skills. Additionally, we are learning that MS disease-modifying therapies may also help MS cognition, which is good news of course for individuals with relapsing forms of MS. However, some medi-cations are now being studied for cognition in individuals with progressive forms of MS, which is certainly good news for individuals with this type of MS as well.”
Cognitive rehabilitation and retraining offers many valuable strategies for achieving goals and attaining optimum quality of life. With this in mind, anyone who believes that he or she may be experiencing changes in cognitive function is encouraged to consult his or her neurologist about the potential benefits that this type of therapy may provide.
RESOURCES
Baumstarck K, et al, “Quantification of relevance of quality of life assessment for patients with cognitive impairment: the suitability indices.” BMC Neurol. 2014 Apr 8;14:78.
Beier M, et al, “Improved physical fitness correlates with improved cognition in multiple sclerosis.” Arch Phys Med Rehabil. 2014 Jul;95(7):1328-34.
Ben Ari Shevil E, et al, “How are cognitive impairment, fatigue and signs of depression related to participation in daily life among persons with multiple sclerosis?” Disabil Rehabil. 2014;36(23):2012-8.
Briken S, et al, “Effects of exercise on fitness and cognition in progressive MS: a randomized, controlled pilot trial.” Mult Scler. 2014 Mar;20(3):382-90.
Catanzaro R, et al, “The gut microbiota and its correlations with the central nervous system disorders.” Panminerva Med. 2014 Nov 12.
Cavallari M, et al, “Microstructural changes in the striatum and their impact on motor and neuropsychological performance in patients with multiple sclerosis.” PLoS One. 2014 Jul 21;9(7):e101199.
Fragoso YD, et al, “The evidence for a beneficial role of vitamin A in multiple sclerosis.” CNS Drugs. 2014 Apr;28(4):291-9.
Francis PL, et al, “Extensive white matter dysfunction in cognitively impaired patients with secondary-progressive multiple sclerosis.” AJNR Am J Neuroradiol. 2014 Oct;35(10):1910-5.
Gingold JN, Facing the Cognitive Challenges of Multiple Sclerosis, Second Edition (Demos Health, 2011).
Gingold JN, Mental Sharpening Stones (Demos Health, 2008).
Jensen H, et al, “Changes in cognition, arm function and lower body function after slow-release Fampridine treatment.” Mult Scler. 2014 Dec;20(14):1872-80.
Jensen, HB, et al, “4-Aminopyridine for symptomatic treatment of multiple sclerosis: a systematic review.” Ther Adv Neurol Disord. 2014 Mar;7(2):97-113.
LaRocca N, et al, Multiple Sclerosis: Understanding the Cognitive Challenges (Demos Medical Publishing, 2006).
McFarland AJ, et al, “Molecular mechanisms underlying the effects of statins in the central nervous system.” Int J Mol Sci. 2014 Nov 10;15(11):20607-37.
Modica CM, et al “Iron and volume in the deep gray matter: association with cognitive impairment in multiple sclerosis.” AJNR Am J Neuroradiol. 2015 Jan;36(1):57-62.
Motl RW, et al, “Walking and cognition, but not symptoms, correlate with dual task cost of walking in multiple sclerosis.” Gait Posture. 2014 Mar;39(3):870-4.
Muhlert N, et al, “Memory in multiple sclerosis is linked to glutamate concentration in grey matter regions.” J Neurol Neurosurg Psychiatry. 2014 Aug;85(8):833-9.
Ozcan ME, et al, “Association between smoking and cognitive impairment in multiple sclerosis.” Neuropsychiatr Dis Treat. 2014 Sep 10;10:1715-9.
Pardini M, et al, “Isolated cognitive relapses in multiple sclerosis.” J Neurol Neurosurg Psychiatry. 2014 Sep;85(9):1035-7.
Pepping M, et al, “Cognition, Cognitive Dysfunction, and Cognitive Rehabilitation in Multiple Sclerosis,” Phys Med Rehabil Clin N Am. 24(2013) 663-672.
Roberg BL, et al, “Speedy eye movements in multiple sclerosis: Association with performance on visual and nonvisual cognitive tests.” J Clin Exp Neuropsychol 2014 Dec 10:1-15.
Rosti-Otajärvi E, et al, “Patient-related factors may affect the outcome of neuropsychological rehabilitation in multiple sclerosis.” J Neurol Sci. 2013 Nov 15;334(1-2):106-11.
Sandroff BM, et al, “Association between physical fitness and cognitive function in multiple sclerosis: does disability status matter?” Neurorehabil Neural Repair. 2015 Mar;29(3):214-23.
Sandroff BM, et al, “Randomized controlled trial of physical activity, cognition, and walking in multiple sclerosis.” J Neurol. 2014 Feb;261(2):363-72.
Sandroff, BM, et al, “Acute effects of walking, cycling, and yoga exercise on cognition in persons with relapsing-remitting multiple sclerosis without impaired cognitive processing speed.” J Clin Exp Neuropsychol. 2015 Feb 6:1-11.
Thelen JM, et al, “Polypharmacy in multiple sclerosis: relationship with fatigue, perceived cognition, and objective cognitive performance.” J Psychosom Res. 2014 May;76(5):400-4.
Utz KS, et al, “Visual search as a tool for a quick and reliable assessment of cognitive functions in patients with multiple sclerosis.” PLoS One. 2013 Nov 25;8(11):e81531.
Weier K, et al, “Cerebellar abnormalities contribute to disability including cognitive impairment in multiple sclerosis.” PLoS One. 2014 Jan 22;9(1):e86916.
