The MS Process
Multiple sclerosis (MS) is a disease of the central nervous system (CNS). The CNS consists of the brain, optic nerves, and spinal cord. With MS, areas of the CNS become inflamed, damaging the protective covering (known as “myelin”) that surrounds and insulates the nerves (known as “axons”). In addition to the myelin, over time, the axons and nerve cells (neurons) within the CNS may also become damaged. MS is thought to be an autoimmune disease, where the body’s own white blood cells, known as lymphocytes, become misdirected and attack the body’s own myelin and eventually the axons.
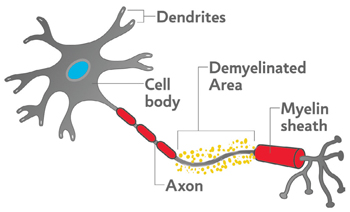
The damage to the protective covering and also to the nerves disrupts the smooth flow of nerve impulses. As a result, messages from the brain and spinal cord going to other parts of the body may be delayed and have trouble reaching their destination – causing the symptoms of MS. Each person with MS may experience different types and severity of symptoms – and some may experience only one or two symptoms, while others may experience a combination of symptoms.
The symptoms of MS range from physical symptoms (such as muscle stiffness, bladder and bowel problems, tremor, and mobility issues), to emotional/ psychological symptoms (such as anxiety, depression, and cognitive changes), to “invisible” symptoms (such as fatigue, numbness, pain, and visual disorders). Please see pages 16-17 for more information on symptoms.
Areas of inflammation and damage in the CNS are known as “lesions.” The changes in size, number, and location of these lesions may determine the type and severity of symptoms. Disease activity may also be evaluated from these changes in the size or number of lesions. Frequently, MS may be “clinically silent,” showing no increase in symptoms, yet continuing to show signs of disease activity within the CNS, as seen on magnetic resonance imaging (MRI) – an important evaluative tool.
 For individuals with relapsing forms of MS, early and continued treatment with a disease-modifying therapy (DMT) can often slow the “clinically silent” disease activity in the brain, reducing the size and number of active lesions. This is one reason why most neurologists recommend that individuals with relapsing forms of MS begin treatment as soon as possible after the diagnosis is established. Treatment may now also be recommended for a portion of those with progressive MS as well as for individuals with clinically isolated syndrome (CIS). However, treatment cannot be effective unless it is taken exactly as prescribed and without missing doses, so adherence is critical.
For individuals with relapsing forms of MS, early and continued treatment with a disease-modifying therapy (DMT) can often slow the “clinically silent” disease activity in the brain, reducing the size and number of active lesions. This is one reason why most neurologists recommend that individuals with relapsing forms of MS begin treatment as soon as possible after the diagnosis is established. Treatment may now also be recommended for a portion of those with progressive MS as well as for individuals with clinically isolated syndrome (CIS). However, treatment cannot be effective unless it is taken exactly as prescribed and without missing doses, so adherence is critical.
In addition to the lesions, areas of thick scar tissue may eventually form along the areas of permanently damaged myelin. These areas of scar tissue are referred to as “plaques.” The term “multiple sclerosis” originates from the discovery of these hardened plaques. Multiple refers to “many;” sclerosis refers to “scars.”
Lesions and plaques are viewed on a magnetic resonance imaging (MRI) scanner. This technology is used to help diagnose MS and evaluate its progress at various intervals. The MRI and other tools are described in the section titled, “Diagnosing MS and Evaluating Disease Activity,” beginning on page 10 of this booklet.
