Types of Multiple Sclerosis
 Multiple sclerosis (MS) affects each person differently. The most common types of MS are:
Multiple sclerosis (MS) affects each person differently. The most common types of MS are:
- Relapsing-Remitting MS (RRMS)
- Secondary-Progressive MS (SPMS)
- Primary-Progressive MS (PPMS)
Initially, most people with MS experience symptom flare-ups, which are also known as relapses, exacerbations, or attacks. When someone experiences a relapse, he or she may be having new symptoms or an increase in existing symptoms. These usually persist for a short period of time (from a few days to a few months) and afterward may remain symptom-free for periods of months or years. This type of MS is referred to as relapsing-remitting MS (RRMS). Approximately 80 to 85% of MS patients are initially diagnosed with this form of the disease.
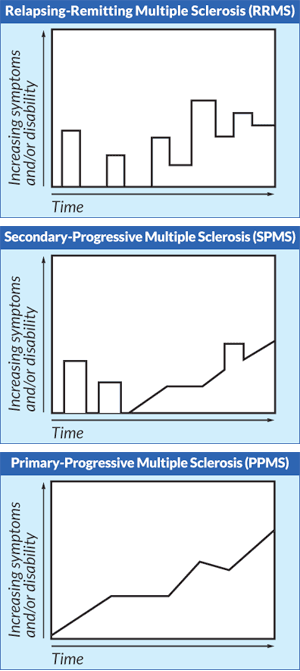 These charts appear in the publication, Primary Progressive Multiple Sclerosis: What You Need to Know, jointly published by MSAA and NMSS.
These charts appear in the publication, Primary Progressive Multiple Sclerosis: What You Need to Know, jointly published by MSAA and NMSS.
Over time, RRMS may advance to secondary-progressive MS (SPMS). This form of MS does not have the dramatic variations in symptoms that RRMS does, but rather has a slow, steady progression. Initially, people with secondary-progressive MS may still experience relapses, although these usually do not fully remit. This is referred to as “active” secondary-progressive MS. Without treatment, many of those with this form of MS eventually experience continued progression of disability without relapses, and this is referred to as “non-active” secondary-progressive MS.
Specifically, without treatment, approximately half of individuals with RRMS convert to SPMS within 10 years. However, with the introduction of long-term disease-modifying therapies (DMTs), fewer individuals advance to this latter form of the disease. Since 1993, more than 20 brand-name and generic DMTs have been approved and are available through prescription. Of these 20-plus medications, all are approved for either relapsing-remitting MS specifically, or for relapsing forms of MS (RMS) that also includes secondary-progressive MS with relapses (active SPMS). Two DMTs, Mayzent® (siponimod) oral tablets and Mavenclad® (cladribine) oral tablets, were approved in 2019. These are both approved for RMS and are the first treatments in recent years to be approved specifically for active SPMS. Mayzent is also approved for clinically isolated syndrome (CIS). Later in 2019, Vumerity™ (diroximel fumarate) oral capsules were approved for the treatment of clinically isolated syndrome (CIS), relapsing-remitting MS (RRMS), and active secondary-progressive MS (SPMS).
Individuals who are not initially diagnosed with RRMS may be experiencing a more steady progression of the disease from the onset. Approximately 10% of the MS population is diagnosed with primary-progressive MS (PPMS), where individuals experience a steady worsening of symptoms from the start, and do not have periodic relapses and remissions. Receiving approval in 2017, Ocrevus™ (ocrelizumab) is currently the only DMT that is approved for primary-progressive MS (PPMS). Given via intravenous (IV) infusion, Ocrevus is also approved for RMS.
A small percentage of individuals are initially diagnosed with a less common form of MS known as progressive-relapsing MS (PRMS). This type of MS steadily worsens from the onset, but symptom flare-ups – with or without remissions – are also present. However, as the different forms of MS are further studied, redefined, and reclassified, the label of progressive-relapsing MS is being used less frequently. Other types of MS exist, but these are uncommon and different terminology may be used. Listed below are these less-common forms of MS.
- “Fulminate MS” is a rapidly progressive disease course with severe relapses within five years after diagnosis; also known as “malignant MS” or “Marburg MS,” this form of very active MS may need to be treated more aggressively than other forms.
- “Inactive MS,” sometimes labeled as “benign,” shows little or no change after 15 years; however, progression may occur at a later time.
- “Burned-out MS” is another type of inactive MS; it is a controversial term used to describe MS patients whose MS progression slows dramatically later in life.
Prior to an MS diagnosis, individuals with “possible MS” may often fall under the parameters of one of two syndromes. The first is clinically isolated syndrome (CIS), where someone may have experienced symptoms of MS for the first time, and an MRI may show evidence of MS, but a diagnosis cannot be confirmed at that time. Disease-modifying therapies are often used to treat CIS in an effort to delay or prevent the eventual diagnosis of MS.
The second syndrome is radiologically isolated syndrome (RIS), which is the term used when someone has an MRI performed for an unrelated reason, and shows evidence of MS on the MRI scan, but does not have any signs of MS symptoms. As with CIS, more evidence will be needed in the future to determine if someone with RIS may be diagnosed with MS.
