Health and Wellness: Exercise for Individuals Experiencing Weakness
By Susan Wells Courtney
Reviewed by Jack Burks, MD
Contributions by Brian Hutchinson, MS, PT and Valerie W. Gibson, PT
Weakness may result from one or more of a number of factors. When weakness is caused directly by MS, it is caused by damage to the nerves and an interruption in the flow of nerve impulses, going from the brain or spinal cord to the affected extremity. Additionally, weakness may result from other impairments of MS, such as fatigue, spasticity, or balance problems. “Disuse” can cause weakness as well, and this is when the symptoms of MS reduce one’s level of activity and movement of an extremity.
Some people with MS will attempt to overcome a weakness problem by trying to aggressively strengthen muscles on their own through exercise and lifting weights. Unfortunately, this may further fatigue the muscles. On the other hand, lack of exercise can cause a muscle to become weaker from disuse. Although this sounds like a no-win situation, a physical therapist can design a program aimed at keeping the affected muscles healthy while avoiding further weakness.
According to Physical Therapist Brian Hutchinson, MS, PT, “Different types of exercise therapies may be used to help strengthen muscles. These include weights, elastic tubing, gravity, and manual resistance through skilled intervention by a physical or occupational therapist. In this latter type of therapy, the therapist provides controlled resistance against the limb being strengthened, while the patient pushes against the therapist.
“When treating MS through exercise, the key is ‘quality of movement,’ versus ‘quantity.’ In other words, how you do the movement is far more important than how many times you do the movement. Individuals with MS need a thorough assessment with a physical or occupational therapist to prescribe the appropriate exercises for strengthening as well as overall conditioning.”
Instruction on how to properly perform the exercises is vital. When exercises are prescribed by an experienced therapist, he or she will include: type of exercise, how long to exercise, how often to exercise, and to what degree of intensity. All of these factors promote safety and success.
Exercise can provide many benefits, including flexibility, strength, and improved health, which-all play a role in-improving weakness.
Hutchinson continues, “Exercising with symptoms of MS is much more complex than just going to the gym. For instance, without the proper instruction, individuals exercising on their own can easily create an imbalance between opposing muscles. One example is when the muscles that surround the ankle are stronger in turning the foot ‘in’ versus turning the foot ‘out.’ This may create movement of the foot ‘inward’ when swinging your leg through while walking. This movement could cause one to ‘land’ on the outside of the foot — increasing the risk to twist the ankle and fall. The same is true when working other muscle groups and this can create a greater risk of injury.
“For patients whose insurance does not cover physical therapy and are unable to afford a professional assessment, other avenues for basic instruction are available. Information on exercising with MS may be found through written pieces and websites, although individuals need to make sure that the source is reliable. Specific educational clinics and one-day programs held by organizations such as MSAA can also provide opportunities to learn and practice successful and safe exercises.
“Regardless of level of ability or disability, everyone should do some type of exercise, preferably at least three to four times weekly. Any exercise program, however, should only be done under the supervision of a medical professional. Those unable to be assessed by a physical or occupational therapist should consult their physician for guidance,” states Hutchinson.

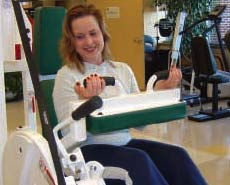
Arm/leg bicycles may be switched to hand pedals for upper body exercise.
Physical Therapist Valerie W. Gibson, PT, is in full agreement with Hutchinson. Gibson comments, “I want to stress the importance of consulting with a medical professional for an evaluation before beginning an exercise regimen. This may be a physical therapist, occupational therapist, or a physician, but these professionals must also have a background in treating MS.”
Gibson continues, “It is important to have an individualized exercise program. Many patients will have different combinations and degrees of symptoms, each requiring a different exercise prescription. Some may have leg weakness while others may have hand and finger problems; some individuals will be ambulatory while others are not; and additional symptoms, including balance, fatigue, and spasticity, contribute to weakness and will need to be addressed as well.”
According to Gibson, the most important exercises are stretching, strengthening, and aerobic conditioning. Stretching exercises should be performed prior to strengthening exercises, and offer several benefits. Stretching decreases the effects of spasticity, increases range of motion (helping joints remain mobile), increases flexibility, and increases blood flow to the muscles and surrounding tissues.
Strengthening exercises will not alter the disease process, but strengthening of the non-affected muscle groups to help compensate for the affected ones, will prevent weakness resulting from disuse. Gradually, strengthening exercises can improve energy and decrease fatigue — and by doing so, can reduce weakness. Muscle groups that have not been affected by damaged nerves should be strengthened as much as possible, but this needs to be done slowly over time. All exercises for individuals with MS need to be minimal to moderate in terms of intensity.

Special stairways help individuals learn to negotiate different-height steps, sometimes with an assistive device. They may also be used for stretching (as shown).
Examples of aerobic exercises for ambulatory individuals include working out on a stationary bike, treadmill, or walking. Water exercise, also known as hydrotherapy, offers the benefits of buoyancy. By reducing the pull of gravity, a person with weakness is able to have greater range of motion while exerting less energy to move the limb. The cooling effect of water on core body temperature may also reduce exercise-induced fatigue. Individuals who are non-ambulatory may be prescribed repetitive upper extremity exercises, Theraband® (elastic) exercises, transfers, and bed mobility.
A thorough evaluation is absolutely essential in creating a prescribed exercise program for an individual with MS. During an evaluation, the following areas need to be assessed:
- Range of motion and flexibility in joints
- Strength
- Tone (muscle tightness or degree of spasticity)
- Fatigue and endurance
- Sensory impairment (sense of touch and other sensations, such as numbness or tingling)
- Visual status
- Balance
- Coordination
- Ambulation and assistive devices being used
- Cardiovascular and respiratory status
- Activities of daily living and independence
- Bed mobility and ability to transfer
- Cognition and perception
- Swallowing and speech impairment
- Employment status
- Psychosocial status (including how the family is adjusting to changes with MS)
- Physical environment, accessibility, community resources
Many of the categories above involve weakness. For example, reduced range of motion, lack of strength, spasticity, and fatigue, all contribute to weakness, as extra effort is required for each movement. When vision, balance, and/or coordination are affected, extra energy is needed to remain upright, so these too can increase weakness. Stress — whether related to home, work, social issues, depression, and accessibility — can deplete available energy and result in weakness.
Developing a treatment plan to treat weakness with MS can be quite complex. In addition to medications which may be used to treat the individual symptoms, many other strategies come into play. Among others, this may include planning, energy conservation, and the proper fit and use of assistive devices; different types of exercises, including those to improve balance and coordination; relaxation exercises to reduce stress; counseling to address depression; and possibly modifications to the home to improve accessibility.
Gibson explains, “Most insurance plans will cover physical therapy provided a specific plan is developed and the participant is making progress. For individuals whose insurance does not cover physical therapy, exercise is still very important. The first step is to have any exercise approved by their medical doctor.”
To follow are some general tips for exercise which Gibson provides for individuals with MS. Please note that before beginning any exercise program, individuals should consult their physician.
- Different types of exercises may be done to improve function in weak muscles. These include “active” exercises (performed independently by the patient), “active-assistive” exercises (patient is assisted either by another person, or patient assists him/herself, such as when using the stronger arm to support the weak one to perform an exercise), and/or “resistive” exercises (using items to provide resistance, such as weights, elastic band, etc.).
- Stretching exercises may be done several times throughout the day to keep muscles limber.
- For non-ambulatory patients, programs may include partial weight-bearing exercises, movement with the help of special standing equipment, and repeating the moves needed to transfer from one spot to another.
- Keep in mind that with exercise and MS, quality is important, not quantity.
- Overexertion can cause a rise in core body temperature, which can temporarily worsen symptoms.
- Following exercise, some muscle fatigue or general fatigue may be expected, but if exercise-induced fatigue continues beyond 30 minutes, the exercise was too rigorous.
- If extremities are difficult to lift, do not add weights.
- If using weights, begin with the smallest weight available, then progress very slowly.
Gibson concludes, “The key to being successful with an exercise program is to make it more enjoyable; this will encourage greater compliance. Even in the general population where MS is not a factor, only one-third of those in an exercise program continue to exercise beyond one year.
“Finding a fitness partner can help to make workouts more fun. Participants need to schedule workouts and make them non-negotiable. Keeping an exercise log or journal to chart progress — noting any new achievements — is a good motivational tool. Progress is typically slow, however, and those working out should be aware of this and not become discouraged.”
Many thanks go to Valerie Gibson and Brian Hutchinson for their assistance with this article. Gibson is a physical therapist and founder of Advanced Physical Therapy and Rehabilitation Center, LLC in Vienna, Virginia, specializing in neurorehabilitation. Readers may visit the center’s website by going to www.aptrehab.com; the center may also be contacted by calling (703) 749-0223.
Hutchinson works as a physical therapist for The Heuga Center, located in Edwards, Colorado, which specializes in education and wellness for individuals with MS. Readers may visit The Heuga Center’s website at www.heuga.org; the center may also be contacted by calling (800) 367-3101.
For more information and resources on weakness, assistive devices, or physical therapy, readers may contact MSAA’s Helpline at (800) 532-7667.
References
MSAA booklet, Multiple Sclerosis, Managing Symptoms, third edition, 2002.
Burks JS, Johnson KP, Multiple Sclerosis — Diagnosis, Medical Management, and Rehabilitation, Demos Medical Publishing, New York, 2000.
Schapiro, RT, Managing the Symptoms of Multiple Sclerosis, fourth edition, Demos Medical Publishing, New York, 2003.
As with all of MSAA’s articles, the information provided is for patient education only. Readers are strongly advised to consult their treating physician or other medical professional before making any changes to their treatment, diet, and exercise regimens, as well as to their activities and/or lifestyle.
